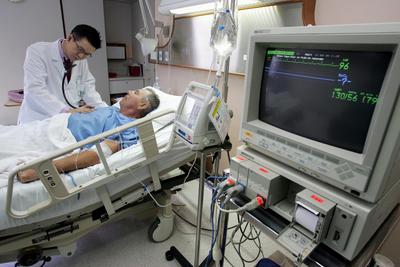
Medical tourism is a practice where patients travel abroad to purchase medically necessary services, such as heart surgeries and hip replacements; elective treatments, such as cosmetic surgeries or reproductive services; and experimental treatments, such as stem cell therapies.
The enthusiastic embrace of medical tourism by East Asian hospitals and governments is, in theory, well justified. Health services exports could potentially diversify regional economies. Industry promoters say it can increase foreign direct investment into the private health sector, help countries retain their existing health workforce, increase training opportunities for health workers, and ensure that the local health sector has access to the latest technological advances. Taken together, these benefits can provide local populations with the opportunity to access cutting-edge and high-quality health services at home.
But medical tourism also creates social and health risks for countries investing in the sector.
Investment in medical tourism can drain resources from the public health sector and divert attention away from the less profitable health needs of the local population. For example, high paying jobs in the medical tourism sector can increase the flow of workers from the public to private sector and from rural to urban areas, as has been the case in Thailand and Malaysia.
New, high-tech equipment and highly trained health workers will certainly be a boon to wealthy patients within these countries. But there is little reason to think that these services, targeted at privileged locals and foreign patients, will be accessible or relevant to the vast majority of the local population. Rather, medical tourism may actively worsen health inequities in these countries. For example, increased investment in the private health sector in India has been accompanied with decreased public sector investment and promised public access to private facilities through public-private partnerships have generally not been realized.
And the promised economic benefits of medical tourism are far from guaranteed. Growth in the sector has come through the lowering of trade barriers in the health services industry. Large regional players in this industry have the power to play governments in the East Asian region off one another, seeking the regulatory and tax environments most favourable to their bottom lines. This competitive environment is doubtlessly favourable to those investing in the medical tourism industry, but it is less clear whether the host countries will experience similar economic benefits if tax concessions and other benefits are not matched by economic returns or if medical tourism developments fail to materialise.
Countries considering marketing their private health sector internationally should be cautious and aware that industry stakeholders have an incentive to inflate numbers about the market’s potential and exaggerate the potential benefits of this industry. As East Asia already hosts some of the most developed and high-profile destinations for medical tourists, it is unclear if new markets in the region can successfully compete for the limited number of medical tourists, especially those from outside East Asia.
If countries do wish to pursue medical tourism development, they should focus on developing the necessary regulatory and healthcare financing conditions domestically that will encourage centres of medical excellence to emerge and prosper. In its worst form, medical tourism is the result of poorly regulated healthcare markets with insufficient domestic healthcare coverage. In these cases, it is likely that medical tourism is primarily a symptom rather than a cause of inequitable and balkanised health systems.
As such, East Asian nations should focus on strengthening or enforcing hospital quality and safety regulations while extending domestic healthcare coverage universally and comprehensively. By focusing on affordability and quality of care, a well-functioning health system oriented to the needs of the local population first and the international market second can develop.
Developing the medical tourism sector in a way that provides sustainable social and economic benefits is a difficult task. Countries in East Asia looking to advance or grow their own medical tourism sectors should be cautious, given that it does not offer a sure prescription for providing economic benefits or addressing health sector ills. Instead, focusing on strengthening core health system elements, such as financing and regulation to improve the quality, affordability, and accessibility of health services locally, may encourage international patients to visit while ensuring that the system is fair and accessible for locals.
Jeremy Snyder, Rory Johnston, Valorie Crooks, Krystyna Adams, Leon Hoffman, and Rebecca Whitmore are members of the Simon Fraser University Medical Research Team.